What causes winter ulcers? The answer isn’t always straightforward. PHARMAQ Analytiq's experts explain why salmon farmers need a holistic, microbiology-led diagnostic approach to address this persistent welfare challenge. It’s also worth noting that the season isn’t over yet—we are still receiving samples positive for winter ulcer bacteria in May—and that the 2025/26 season appears to have started later than usual, with sample volumes increasing only after the New Year.

Moritella viscosa is the bacterium most often associated with winter ulcers in Scotland. It penetrates the skin surface, forms a biofilm on the scales and produces toxins that destroy surrounding tissue, leading to deep ulcers. Other bacteria then thrive in the ulcers.
The disease is complex and poses a serious challenge for salmon farming, causing fish suffering, mortality, and reduced harvest quality. So how should farmers investigate the lesions?
The season isn’t over yet. We are still receiving samples positive for winter ulcer bacteria in May, and the 2025/26 season appears to have started later than usual, with sample volumes increasing only after the New Year—likely linked to seawater temperatures.
Chris Matthews, fish veterinarian and Business Unit Director at PHARMAQ Analytiq UK, warns against relying on PCR alone in winter ulcer diagnostics. Many farmers choose PCR for its speed, but it only tells part of the story.
“While PCR is excellent for speed and sensitivity, it’s essentially a yes/no detector for DNA. It cannot tell you if bacteria are alive, how they are behaving, or if your current vaccines are a good match for the specific strain on that farm. With Moritella viscosa, we need it in culture to understand its phenotype.”

Matthews recommends a holistic diagnostic approach, starting with microbiology – which helps reveal the full range of bacteria present in ulcers.
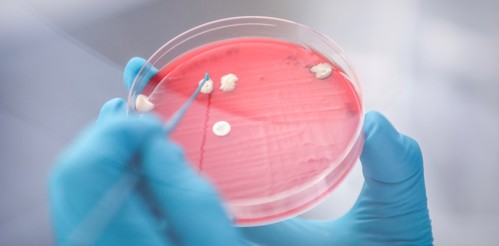
Microbiology requires living bacterial samples. Matthews recommends sampling both the ulcer and internal organs such as the head kidney, to check whether the bacteria have spread inside the fish. Samples should be plated onto fresh agar on site and kept cool during transport to the lab.
In the lab, microbiologists culture the living sample material and study bacterial growth over time. They observe the physical appearance of each colony, noting the characteristics: if it’s raised or flat, smooth or rough, haemolytic or transparent. These descriptions enable microbiologists to identify different variants and subtypes.
Microbiology also works well alongside other diagnostic methods. "You can supplement with PCR to rapidly confirm specific findings, or with histopathology to examine tissue changes more closely," says Matthews.
While winter ulcers frequently involve bacteria such as Moritella viscosa, Tenacibaculum and Aliivibrio wodanis, the external environment plays a significant role in their development.
“Fish are likely frequently being exposed to these bacteria, which are a natural part of the bacterioplankton of seawater, but the pathogen is held at bay by a healthy immune response and the protective mucus layer which overlies the skin,” Matthews says.
“Low temperatures are known to upregulate many of the virulence mechanisms in Moritella viscosa, and in cold temperatures the fish’s immune response is lower – so the balance is tipped in favour of the pathogen’s ability to form an ulcer.”
In recent years, advancements in delousing technology have allowed the industry to move away from chemical treatments for sea lice. However, increased physical handling events increase the chance of micro-abrasions to the skin, Matthews explains.
“Despite appearing to our eye to be surface structures, scales in healthy fish are in fact protected by a layer of skin known as the epidermis. Micro-abrasions to this delicate structure expose scales and make it easier for ulcer-forming bacteria to establish.”
This complexity underscores why Matthews advocates a holistic diagnostic approach.
Winter ulcers are usually easy to recognise on site, but fish health teams should always consider whether the lesions could have a different cause.
“In rare cases, piscirickettsiosis or even ruptured furunculosis lesions have been misidentified as winter ulcers. Moritella viscosa can even return a weak positive on PCR in such cases, without actually being responsible for the lesions,” cautions Matthews.
Occasionally, no pathogenic bacteria are present in a case at all, which might point to other infectious or non-infectious causes, explains Matthews.
Winter ulcers in Scotland were historically caused by the ‘classical’ strain of Moritella viscosa, and the first commercial vaccines available protected against them. Over the past decade, ‘variant,’ and more recently ‘non-viscous classical’ strains have become dominant. The earlier vaccines do not cover these.
“The vast majority of Moritella viscosa cases in Scotland are now caused either by variant or non-viscous classical strains, and occasionally we find both present in the same cases,” says Matthews.
PCR can distinguish between some of these forms, but not all. The non-viscous classical form can only be identified through microbiology.
“Only by culturing the bacteria can we definitively characterise the strains present through assessing their phenotype and understand whether available vaccines cover these.”
Culturing bacteria also offers several long-term advantages, Matthews notes.
“While antimicrobial treatments for winter ulcers are rare, only by culturing bacteria can antimicrobial resistance testing be undertaken.”
Bacteria cultured for microbiological investigation are stored in a biobank at - 80 °C. The biobank can be used to develop new vaccines, monitor how bacteria change over time or conduct research.
For Tenacibaculum, no commercial vaccine currently exists. The biobank is therefore especially valuable.
"The more isolates you have available, the better. What we do this year could lead to drastically improved fish health in just a few years," says Matthews.
Microbiological investigation can complement PCR and help build a more complete diagnostic picture. PHARMAQ Analytiq recommends collecting a complete set of samples when investigating a disease problem.
“The most costly outcome is having to take new samples. When you’re already there investigating a disease problem, take a complete set of samples and send them for microbiological analysis. Then you avoid having to submit samples again,” says Matthews.

There are multiple types of winter ulcers, each associated with different bacteria.
Classical winter ulcers are primarily caused by the bacterium Moritella viscosa. The bacterium attacks the skin and can also infect internal organs such as the head kidney, spleen, liver and bloodstream – known as a systemic infection. Three forms of Moritella viscosa have been identified: classical, variant and non-viscous classical.
Atypical winter ulcers are associated with the bacterium Tenacibaculum. The infection causes surface lesions and tissue decay around the jaw, head and fins.
The bacteria can occur individually or together. Other bacteria, such as Aliivibrio wodanis and Vibrio splendidus, are also frequently detected in winter ulcer lesions. Researchers are still working to map the exact roles these different species play in outbreaks.
PHARMAQ is the global leader in vaccines and innovation for aquaculture and part of Zoetis, the world leader in animal health. The company provides environmentally sound, safe and efficacious health products to the global aquaculture industry through targeted research and the commitment of dedicated people. Production facilities, administration and research and development activities are based in Norway with subsidiaries in Chile, United Kingdom, Vietnam, Turkey, Spain, Panama and Hong Kong. PHARMAQ has approximately 300 employees. The company's products are marketed in Europe, North and South America, and Asia. For further information, visit the company's website at www.pharmaq.com. Privacy Policy. Cookie Policy. Terms of Use.
Copyright © 2020 Zoetis LLC. All rights reserved.